Understanding MND
“Perseverance is not a long race; it is many short races one after the other.” – Walter Elliot
Types of MND
There are several major types of MND
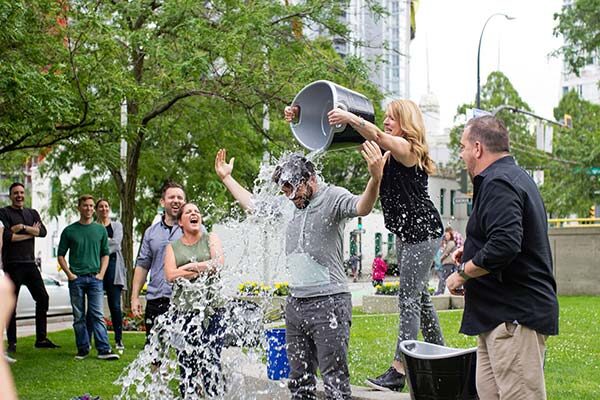
Amyotrophic Lateral Sclerosis (ALS) :
ALS or Lou Gehrig’s disease is the most common type of MND. You might have probably heard of it in passing at least from the ALS ice-bucket challenge that trended on social media a few years ago.
“Myo” means muscle and “Trophic” means nourishment and “A” in the beginning denotes “no”. Thus, Amyotrophic means no muscle nourishment. Lateral means “to the side of”. It denotes where the damage occurs. Finally, “Sclerosis ” refers to the hardening of the tissue. It is also called Lou Gehrig’s disease after a famous American baseball player who had the disease.
ALS typically affects both upper and lower motor neurons. Due to muscles not receiving signals from the nerves to contract, they waste away. This is called “atrophy”. It primarily affects the muscles on the arms, legs, mouth, and respiratory system. Symptoms depend upon the area being affected, however, general symptoms are muscle wasting, stiffness, weakness, cramps, “fasciculations”(twitching), etc. It generally affects one side of the body first, however as it develops it becomes symmetrical on both sides.
We do not know why it occurs and neither do we have a cure. Treatment can improve the quality of life and helps address symptoms. It can be inherited, but in most cases it is sporadic. Those affected tend to live between 3-5 years but with proper supportive treatment and care, patients have lived more than 10 years as well.

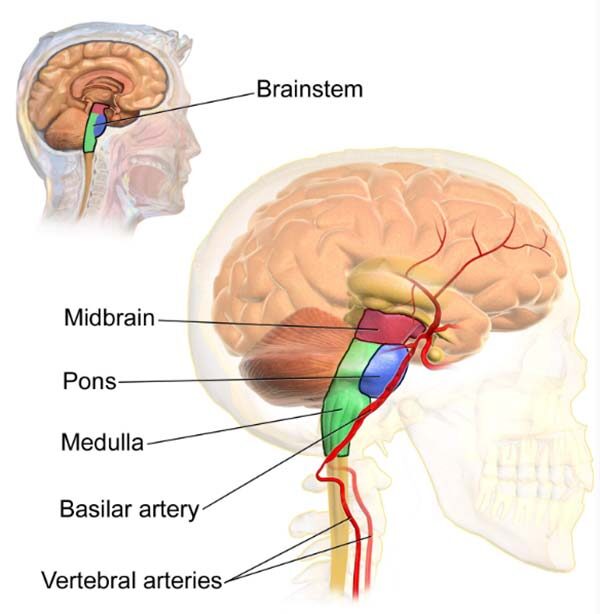
Progressive Bulbar Palsy:
“Bulb” is the old way of referencing the brain stem, which is the area affected with Progressive Bulbar Palsy. It damages the motor neurons within the brain stem, which is located at the base of the brain. PBP eventually progresses into ALS, which is why it has “progressive” in the name.
The brainstem helps us chew, swallow and speak. Thus, all these actions are affected and slurred speech is commonly seen in PBS. Furthermore, emotions also become hard to control, with laughter and crying becoming out of the person’s control. Pseudo-Bulbar Palsy and Mixed-Bulbar Palsy also affect the brain stem and showcase these symptoms.
As PBP affects the lower motor neurons, there tends to be atrophy of the tongue and fasciculations. Speech becomes “nasally”. In the case of Pseudo-Bulbar Palsy, the upper motor neurons are affected, thus tongue spasms and stuttering are symptoms.
Progressive Muscular Atrophy:
This affects the lower motor neurons and is rarer than ALS and PBP. Muscle weakness and cramps, especially in the hands, are quite common in this MND. There is also a loss of weight, lack of reflexes, and muscle twitching. If it spreads and affects the upper motor neurons as well, then it is re-classified as ALS.
Progressive Muscular Atrophy has a comparatively slow rate of progression and typically those affected have a longer lifespan than ALS and PBP.
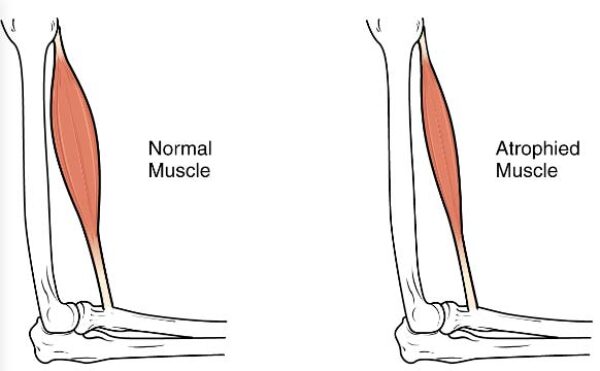
Primary Lateral Sclerosis:
PLS affects the upper motor neurons in the legs, arms, and sometimes the face. The motor neurons in the upper layer of the brain (the cortex) degenerate, leading to spasticity (stiffness) that increases over time. It usually starts affecting lower limbs, then spreads to the upper body, and finally affects the bulbar muscles (thus affecting speech, chewing, swallowing, etc.).
Progression typically takes a long time, however, this might vary on a case-to-case basis. It is also not fatal, some people affected might still be able to walk even when the disease has progressed. However, this is not the case for everyone, as others might need assistive devices for mobility.
Post-polio Syndrome:
There is a lot that is unknown about this disorder, especially regarding what causes it. What we do know about it is that it affects survivors of Polio often decades after their recovery. Polio is caused due to a virus that spreads from person-to-person contact. The disease can manifest in different ways with some developing flu-like symptoms, others getting meningitis, and others developing the most severe symptom-paralysis.
Unlike Polio, Post-Polio Syndrome is not contagious. This can develop even in those who have completely recovered from Polio, often 15-40 years later. When Polio first attacks the body, motor neurons are affected, which leads to the surviving neurons enlarging and sprouting new dendrites. However, this puts the motor neurons under stress and eventually they deteriorate again- which is believed to be the cause of PPS. It is commonly not life-threatening, however progressive muscle weakness, fatigue, atrophy, etc. can make mobility difficult. In cases where it has affected the bulbar regions, it can lead to difficulty chewing and swallowing and if it leads to muscle weakness in the chest it can result in breathing issues.
Additionally, there are also other muscular diseases that do not involve motor neurons. However, they have similar or overlapping symptoms to MND and often use the same therapy and treatments. Thus, we will be including a few of those under this section as well.
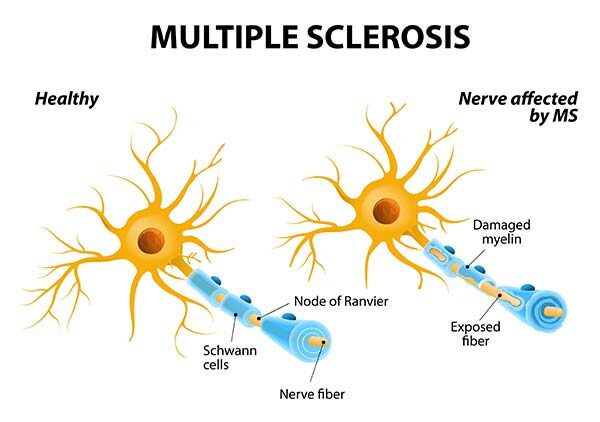
Multiple Sclerosis:
Multiple Sclerosis is an autoimmune disorder that causes the body to attack its own cells- specifically the CNS of the brain and spinal cord. The myelin sheath that protectively coats the nerve cells is destroyed, which slows the transmission of signals from the brain to the body. This leads to a weakening of muscles and motor coordination becomes difficult. Other symptoms are spasms, stiffness, fatigue, slurring of speech; all similar to ALS. Due to this overlap of symptoms, MS and ALS are often confused with each other-especially in the early stages. As both diseases progress, the symptoms vary.
Since there is no single test to determine either disease, the only way is to rule out other possible disorders is through a study of the medical history along with diagnostic tests and examinations. While ALS is a rapidly and progressively deteriorating disease, this is not the case with MS which has a different timeline in each person. Sometimes symptoms show early on and in other cases, they only develop towards later stages. Due to this, it is not easy to predict how fast the progression will be, what symptoms can occur, or how severe they will be.
It is not a fatal disorder and most people can expect normal or close to normal lifespans. Unlike in the case of ALS, Multiple Sclerosis can impair mental capabilities and sensation. Due to the myelin sheath being scarred and damaged, the sensory nerves have trouble relaying information. Although mobility is affected, it is usually not completely debilitating. In the later stages, there can be significant impairment of sight, bowel movement, emotional health, cognitive abilities, etc. There is no cure, however, timely treatment to manage symptoms is vital for the person to have a good quality of life.
Myasthenia gravis:
This is an autoimmune neuromuscular disease that results in the body blocking certain receptors in its neuro-muscular junctions (the point where the nerves meet the muscle). This affects the communication between the nerves and the muscles, which in turn affects muscle contractions and leads to weakness. The weakness gets worse during periods of activity and improves when the patient rests. Myasthenia gravis affects the voluntary muscles of the body, especially those that control the eyes, mouth, throat, and limbs.
A majority of patients show “ocular symptoms” a.k.a symptoms that affect the movement of the eyes and eyelids along with the generalised weakness. Ocular symptoms can include double vision, droopy eyelids, trouble focusing, etc. The generalised weakness can also develop after the ocular symptoms show up.
There might be other symptoms as well such as issues talking and walking, facial paralysis, difficulty swallowing, hoarse voice, etc.
Myositis:
Myositis is a general term used to refer to inflammatory myopathy. It literally translates to “muscle inflammation” and this is commonly due to an autoimmune issue- although it can even be caused through injury or infection as well. This presents two major types of diseases- polymyositis and dermatomyositis. Both these diseases are more prevalent amongst women and generally occur during adulthood. Polymyositis begins with muscle weakness, especially in the trunk of the body which spreads over time. Dermatomyositis also has similar symptoms, along with a purple rash.
Myopathy
This is a general term used for neuromuscular disorders that are caused due to dysfunction of the muscle fibres. This can either be inherited, or acquired later in life. Inherited myopathies have an earlier onset and a longer duration when compared to the acquired ones. They can be acquired due to auto-immune issues, toxins, infections, hormonal issues, and other systemic issues (such as electrolyte problems, steroids, etc.).
Inherited myopathies include muscular dystrophy, congenital myopathy, metabolic myopathy, and mitochondrial myopathy- all of which have several specific types of diseases underneath these categories. We will be looking at a few major types of myopathies below.
Muscular Dystrophy:
This refers to a group of inherited disorders that leads to a progressive degeneration of muscles which leads to muscle weakness. This is caused due to the lack of a protein called “dystrophin” that helps strengthen and protect muscle fibre. The absence of dystrophin can cause issues in walking, swallowing, and coordination of the muscles. The most common of these disorders is Duchenne Muscular Dystrophy, which has an early onset around ages 2 and 3. It tends to affect boys more than girls. With the latest advancements in treatments, those affected with Duchenne might live well into their 30s, even with an early onset of symptoms. The disease most usually progresses to the extent that a wheelchair becomes necessary.
Becker Muscular Dystrophy is not as intense, with symptoms showing up later in childhood and progressing more slowly. A wheelchair only becomes necessary in the latter part of their thirties and the forties- some people will not even have to use one.
There are several other dystrophies, with varying severity of symptoms and progression.
Image Source: Wikimedia & Unsplash

 Dr. Alexander Thomas | President, AHPI
Dr. Alexander Thomas | President, AHPI
